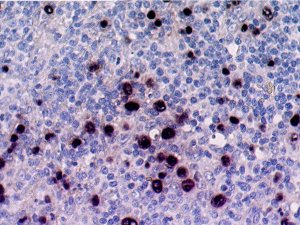
Epstein-Barr virus-encoded RNA (EBER) demonstrated by in-situ hybridisation in a case of post-transplant lymphoproliferative disease.
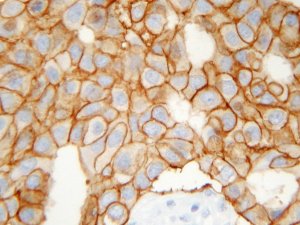
Over expression of HER2, a member of the erbB epithelial growth factor receptor family in a breast carcinoma case.
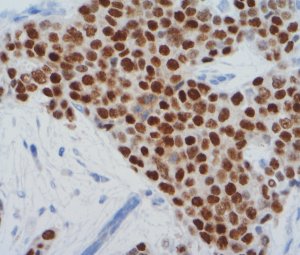
An oestrogen receptor positive breast carcinoma.
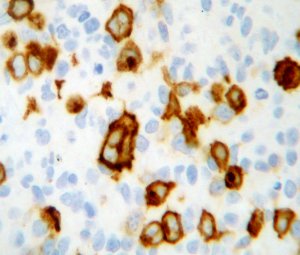
CD30 positive Reed-Sternberg cells in a case of Hodgkin's disease.
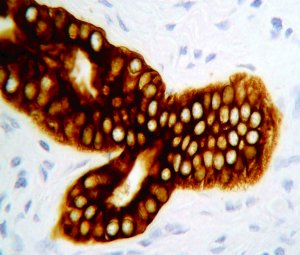
A normal duct, the epithelial cells of which have been stained using an antibody to cytokeratins (an intermediate filament protein).
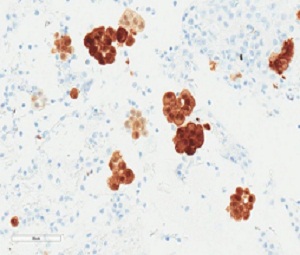
Groups of mesothelioma cells in a non-gynae cytology EBUS specimen which have been stained using an antibody to calretinin (which is expressed in both normal and neoplastic mesothelial cells and is a useful marker for the identification of malignant mesothelioma of the epithelial type).